Last week, I wrote about a realization that had suddenly come to me. I was intrigued (and dismayed) by a series of unrelated and spontaneous public acts of interpersonal violence: a fan brawl at a baseball game; a player brawl at the same stadium a day or two later; a Cardi B fan throwing a drink at her as she sang, prompting Ms. B to hurl her microphone right back at him; and hundreds of teens rioting in a New York City park over… whatever. Motive doesn’t seem to matter.
What first caught my attention was the sudden and seemingly unprovoked nature of those attacks. It was as if all those people had little, or no, control over their emotions. They were all fight and no flight.
That’s when the thought occurred to me: the volatile actions of those people felt similar, in many ways, to the emotional dysregulation people with a number of mental disorders experience. These include BorderIine Personality Disorder (BPD), also known as emotionally unstable personality disorder (EUPD). The U.S. National Institute of Mental Health (NIMH) describes BPD as “a mental illness that severely impacts a person’s ability to manage their emotions. This loss of emotional control can increase impulsivity, affect how a person feels about themselves, and negatively impact their relationships with others.”
Please note
As I stated in Part 1 of this thread, I am not equating the experiences of people with BPD to the social miscreants attracting attention due to their inexcusable behaviors. I am certainly aware there are many other difficult aspects of living with BPD, but I could not help noticing that when certain specific parts of the brain become physically corrupted and dysfunctional, emotional dysregulation can and does occur.
There are two areas of the brain that are particularly involved in the disruption of emotional stability: the amygdala and the pre-frontal cortex.
The Amygdala
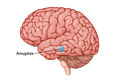
The amygdala is a walnut sized organ located near the base of the brain that is part of the what is known as the limbic system, a group of structures that, among other things, help regulate emotional responses and related behavioral actions.
The amygdala generates the familiar fight or flight response. It also serves a variety of purposes such as fear conditioning, processing positive emotions and creating emotional memories.
The Prefrontal Cortex (aka PFC)
The PFC is the area of the brain where information from the amygdala, like fight or flight impulses, are further processed, evaluated and acted upon. This is where ‘executive function activities such as decision-making, planning and emotion regulation occur.
What’s the connection to BPD?
A research study published in the journal Neuropsychopharmacology noted that:
Borderline personality disorder (BPD) is an illness, characterized by the symptom of emotional dysregulation and disinhibited anger, which often leads to aggressive behavior. The model of altered prefrontal–amygdala connectivity provides a model for the primary symptom in BPD, disinhibition of emotion.
Doctor Antonia New, a psychiatrist and BPD researcher at the Mt. Sinai Medical School in New York, was the principle investigator for that study:
What Causes the PFC to Deteriorate?
To answer this, we need to go back to the amygdala. The amygdala is the input center for sensory information coming from from the world outside the body. Signals from our sensory organs - eyes, ears, mouth, nose, skin- are transmitted via the nervous system to the amygdala for instant analysis and action.
When dangerous threat is detected, the “fight or flight” response is automatically triggered. A flood of hormones such as adrenaline and cortisol are released to prepare the body for emergency action. This ‘stress’ response causes physical changes such as a faster heart rate, raised blood pressure, quicker breathing and tightening of muscles, increase strength, speed up reaction time, and enhance focus, all in preparation to fight or flee. And it all happens in seconds.
Stress And The Amygdala Hijack
This is a term created by psychologist and author Daniel Goleman in his book “Emotional Intelligence”. It refers to an emotional reaction to a threat that is out of proportion to a situation that is not actually dangerous enough to warrant an all out alarm.
Chronic stress can cause the amygdala to build up it’s supply of neurons that connect it to the PFC and other brain areas. Over time, the amygdala grows in size and capacity to meet the perceived higher levels of stress. Brain imaging involving people who have BPD reveal an enlarged amygdala, giving it more ‘bandwidth’ to send information to the PFC.
Paradoxically, this hyperactivity has a negative effect on the PFC. It causes cell loss, corrupting the way the PFC functions, diminishing its ability to manage high levels of emotional reactivity. Thus the term ‘amygdala hijacking' - when the amygdala is over activated, the prefrontal cortex is less activated.
When emotions run high, blood and oxygen flow to the amygdala rather than the prefrontal cortex, the PFC loses calls and effects our ability to think and solve problems when a person is highly stressed.
So, chronic stress weakens the structures (PFC) that provide negative feedback on the stress response and strengthens the structure (amygdala) that produces the stress response.
This is, of course a time of very heightened stress in nearly all our lives. Social stress, covid isolation and separation, schools and workplaces closed, masks, fear of contact, fear of sickness and death, climate and environmental stress. Evidently we now have to worry about space debris falling back into earth’s atmosphere and surface.
What Can We Do?
Actually there are a number of suggestions and strategies, from psychological therapies to old fashion common sense, that can help reduce stress.
In the third and final episdoe of this thread we will review what stress releiving interventions are available, how they work and how to access them.
In the meantime, knowing there is help might reduce some of your stress..