The government will kick millions off of health insurance soon
KFF estimates that 5 million to 14 million will lose Medicaid coverage
Since the start of the pandemic, Medicaid, the health insurance program for low-income Americans funded by the feds and the states, has been far more generous than in the past and seen an all-time high in enrollment. It is now the largest single source of coverage in the US. Over 90 million people rely on Medicaid and its related children’s health program for their coverage. Approximately 41 million of these people are children – at least half of children in the United States are now covered through Medicaid.
Millions of Americans got health insurance coverage through Medicaid during the pandemic — coverage that many otherwise would not have been able to find elsewhere. And starting in April of this year, thanks to Congress, millions of Americans will lose that coverage. Some will be able to get covered in other plans, but others are bound to fall through the cracks and become uninsured.
Some context:
Under the Families First Coronavirus Response Act (the first coronavirus relief bill passed in March 2020) states received a 6.2 percent boost in federal Medicaid funding in exchange for halting disenrollments. States were unable to kick anyone off of their Medicaid programs as long as the federal government’s designation of the public health emergency (PHE) was active.
In a normal year, many people enroll in Medicaid and many others leave as their income or circumstances change. States would run routine checks on Medicaid members to make sure they're still eligible for the program, and throw out anyone who wasn’t. The public health emergency halted that process.
But the $1.65 trillion omnibus bill which was recently signed into law allows states to kick people off of Medicaid starting in April of 2023, even if the PHE remains active. States can take up to a full year to initiate all renewals of coverage for Medicaid recipients.
What this means:
The Kaiser Family Foundation estimates that 5 million to 14 million people will lose Medicaid coverage during the 12-month unwinding period. Many will find coverage elsewhere, but not everyone. A December study by the centrist Urban Institute estimated that 3.8 million will end up uninsured as a result of the purge.
Public-health advocates are concerned that the overwhelming amount of eligibility redeterminations will result in people losing Medicaid coverage even if they are eligible. They also worry that people will wind up uninsured because they don’t know about their eligibility for other coverage, such as employer-sponsored health insurance or Affordable Care Act plans.
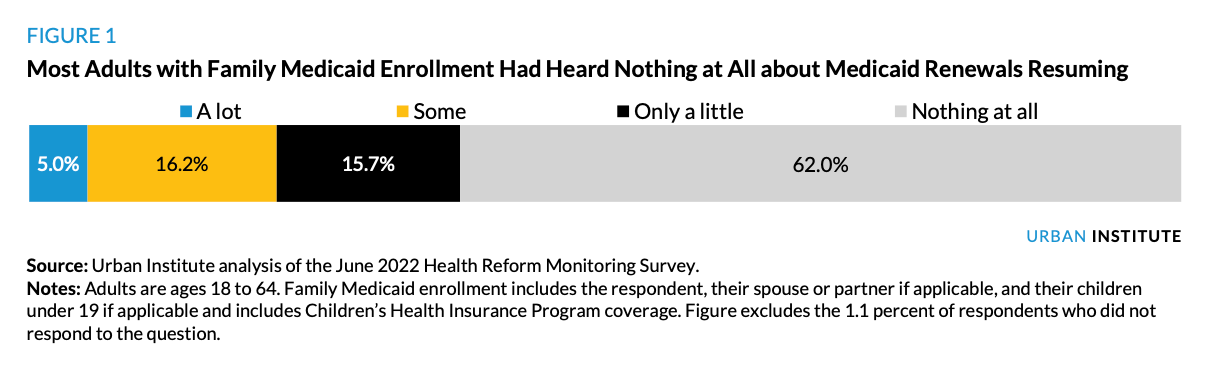
They have good reason to worry: the government hasn’t been doing a particularly good job of informing people of this forced transition. Back when the feds said that states can’t kick people off of Medicaid while the PHE is active, most adults with family Medicaid enrollment had no idea of the looming return to regular Medicaid renewals.
Out of those who had heard about the upcoming purge from state agencies or health plans, most of them say that they never heard about other coverage options available to them if they become ineligible for Medicaid, or how to get assistance with the renewal process.
I’m willing to bet that people have not gotten more informed about this incoming disaster where the circumstances have slightly changed, but the end result hasn’t: even if the PHE remains active, millions will become uninsured.
If you’re in Massachusetts like me, The Health Care For All HelpLine is a free multi-lingual statewide resource to help consumers with health coverage. When I turned 26, the transition from my parents’ health insurance coverage to MassHealth was extremely bumpy and extremely stressful. I wish I had known about that number sooner.