How to Turn Injury into Opportunity
What osteoporosis (and other skeletal woes!) can teach us about our mental & physical health
March Madness is wrapping up! So this week is all about skeletal health.
Today’s newsletter (below) is about osteoporosis—and how a skeleton on the FRITZ can affect our whole health ecosystem.
Today’s podcast is a solo episode about the lessons learned from physical injuries that sideline us from everyday activities (with a bit of my own history sprinkled in). Listen here!
For this Friday’s Q&A, I welcome your questions about skeletal health. Submit your questions here.
Join me for our next Zoom hangout on Wednesday April 19 at 8 pm ET! We will discuss The Four “I”s, i.e., the framework I use to conceptualize health You can register here! This is for paid subscribers only.
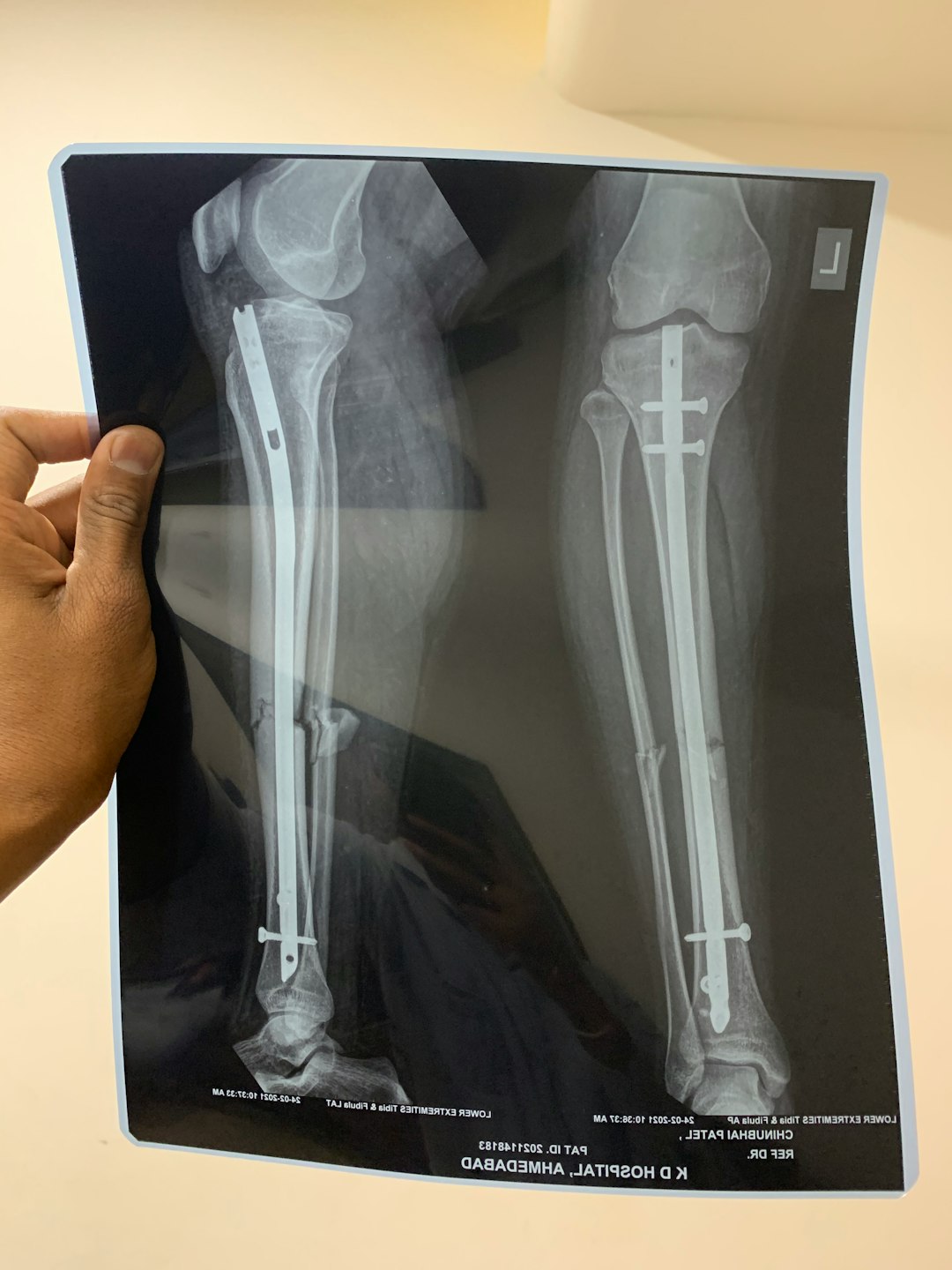
I recently saw a 62-year-old patient who fell and broke her leg. Two weeks prior to our visit, she tripped over her dog’s leash and landed in a heap on the pavement in front of her house. She came in to see me to discuss her osteoporosis, which predisposed her to fractures, and her despair over her inability to exercise for many months.
I feel like I’m falling apart! I don’t like feeling old!
These were some of the G-rated musings that she blurted out as she hobbled into my office.
During our conversation, she expressed remorse that she had declined my recommendation the year prior to start taking weekly Fosamax to help prevent fractures. Like many of my other patients, she had been worried about side effects. She admitted that she had been put off by the horror stories she had read online—plus the consternation from friends when she broached the subject.
It turns out she is not alone. Osteoporosis is a major health concern in the US, where an estimated 10 million individuals have osteoporosis and another 44 million have low bone density, which puts them at increased risk for the disease. Osteoporosis-related fractures are responsible for an estimated $19 billion in healthcare costs annually, and the incidence of these fractures is expected to rise as the population ages.
She’s also not my only patient whose adventures on Google do harm. I spend a fair amount of time with patients helping them fact-check strongly held beliefs about certain medications, especially when they gain a reputation of causing more harm than they actually do. I often find that undoing fear-based headlines is like trying to stop a 747 in its tracks. (See also: hormone replacement therapy, COVID policies re: children.)
Women are particularly vulnerable to osteoporosis, with 1 in 2 women over the age of 50 experiencing a fracture due to osteoporosis. Age, genetics, and hormonal status are some of the risk factors. Indeed, osteoporosis is one of the potential “side effects” of menopause; conversely, hormone therapy can help prevent it.
Men can also develop osteoporosis, particularly those with a family history, low testosterone, low body weight, celiac disease, and other predisposing medical conditions. Younger women can develop osteoporosis, too, if they experience amenorrhea (loss of their menstrual cycle), low body weight, or premature ovarian insufficiency (POI).
Adding insult to injury, our balance naturally declines as we age and is exacerbated by inadequate muscle tone (in addition to poor eyesight, foot problems, medication side effects, and other issues). Falls are the leading cause of injury and death-related injury in Americans over 65. Deaths related to falls have increased by 30% in the past decade.
But health is about more than treating the physical symptoms of a condition. It is about taking a holistic approach to wellness and recognizing that we are the integrated sum of complex parts. Health is about having awareness of data and the stories we tell ourselves, acceptance over the things we can't control, and agency over our life.
My advice to my patient?
Awareness of the data and the stories we tell ourselves
To validate my patient’s feelings of feeling frustrated and “old”—and to give herself permission to be human. “It’s normal to be aggravated when we blow a gasket!” I reminded her.
To understand how easily the morass of medical information on the internet (and well-intended friends) can generate anxiety and inadvertently steer us away from relevant medical data and facts.
To recognize that the side effects of bisphosphonates (i.e., Fosamax, Boniva, and its kin) are exceedingly rare. The more common (although still rare) side effects of stomach upset or heartburn usually can be mitigated by appropriately administering the medicine.
Acceptance
To work on the painful process of accepting her temporary disability—and to use it as an opportunity to self-reflect: What kinds of movements and activities are most meaningful in my life? What are the things I expect from my skeleton—and how can I care for it like it takes care of me? (See my short solo podcast below.)
Agency
To begin taking Fosamax to help prevent further fractures. There are several classes of medications available to treat osteoporosis, including bisphosphonates, denosumab, and teriparatide. Bisphosphonates such as Fosamax and Boniva are among the most commonly prescribed medications for osteoporosis. They work by slowing down the activity of the cells that break down bone tissue, which helps to maintain bone density.
To call me if she has any side effects! Cultivating open communication with patients is critical to the success of any intervention.
To focus on strength and muscle mass in order to help prevent and treat osteoporosis. Regular weight-bearing exercise, such as walking and lifting weights, can help to build and maintain bone density. How much weight training does one really need? Amazingly little. Even twenty to thirty minutes twice a week is enough to make a significant difference in strength and, as a result, bone density.
To eat a diet that is rich in calcium and vitamin D. I prefer that patients get calcium through diet (ideally 1000-1200 mg daily)—though I’m not against supplementation if their intake is low.
For her emotional distress, to seek out alternative forms of exercise that she could do while recovering, such as gentle yoga or water aerobics. Yoga gets all of our major muscle groups. It’s also great for balance, flexibility, and mindfulness.
To connect with her friends and loved ones to discuss her feelings of helplessness. The social isolation from physical injuries is real!
To ask for help. For example, instead of proudly declining neighbors’ offers to bring dinner, to accept them—and to admit that she needs the added support.
And, ultimately, to treat her skeleton like the vehicle that it is. We only have one vehicle to drive us through life!
Health is always about tradeoffs. Treating a patient’s osteoporosis is about balancing the potential risks of medication with the potential risks of fractures and associated disability, all the while caring for the whole person inside.
In today’s solo podcast, I discuss the importance of caring for our skeleton like we do our cars—taking it to the shop when it breaks down, and providing regular maintenance.
I give three examples of people whose physical injuries forced them to reckon with their health—a college athlete with knee problems, an older man with arthritis, and me in my 20s!

Our skeletons provide the structural integrity for our everyday health. They allow us to walk the dog, open jars, play bridge, and lift grandchildren. It’s easy to take our skeletons for granted. How do you care for yours? What can an injury teach you about your health? What is the relationship, for you, between mobility and mental health?
Disclaimer: The views expressed here are entirely my own. They do not reflect those of my employer, nor are they a substitute for advice from your personal physician.
To support this work and for lots of fun extras, consider a paid subscription!




I liked what you said about “calling your doctor” when you have questions. It would be great if we could do that. The doctors I have had in recent years are protected by so many layers of screening. If I’m persistent I can get a nurse but I rarely get to talk to my drs on the phone. I spent a whole career of 40+ years as a public school teacher and administrator. I know how important personal contact is to good communications. Why are doctors so afraid of it? Even when I get through and leave my question, it is the nurse who returns my call and often several days after it was asked. Just blowing off some steam! Thanks for a great column. I don’t miss any of them and I hope to sit in on one of your Zoom sessions soon.
Have spent several sessions in Neuro Balance Center @ Kettering Health Network.
Especially careful after reading obituary of way back friend Astronaut Walt Cunningham. Death “results of a fall” at 92.