Endometriose e estrogênio - o problema e sua causa
Estrogênio, especialmente estradiol [E2], constrói e alimenta a endometriose
[Imagem: smclinic-spb.ru]
Os artigos científicos abaixo citados fundamentam várias ideias sobre a endometriose – sua fisiopatologia – que são pouco focadas pela medicina dominante e que, se devidamente avaliadas e levadas a sério poderiam promover uma revolução na estratégia de tratamento da endometriose.
Poderiam trazer a progesterona para o centro de qualquer planejamento consequente de abordagem dessa doença que tanto mal e sofrimento causa a milhões de mulheres mundo afora, tanto antes quanto depois da menopausa. Progesterona e tireoide.
A medicina, em grande medida, já sabe que a endometriose é causada por excesso de estrogênio, tanto que em alguns lugares se utiliza inibidor da enzima que sintetiza estrogênio [aromatase ou P450arom] no tratamento da endometriose.
Mas, novamente, ela se guia pelas aparências e, ataca o que vê pela frente, com drogas tóxicas [inibidores da aromatase] quando poderia lançar mão de poderosos e fisiológicos inibidores da aromatase, como progesterona e pregnelolona.
A medicina oficial também sabe que quando suspendem aquelas drogas anti-aromatase, a endometriose costuma voltar, portanto não se trata de cura. E, pior, lança mão, com frequência de métodos sobremaneira agressivos contra a endometriose como cirurgia e até aniquilação do ovário, na ânsia de diminuir o estrogênio corporal. Com isso não apenas não garante a cura como também mostra o quanto está às cegas diante do do problema. E também uma preocupação duvidosa, pouco convincente em relação, de fato, à saúde da mulher, sua qualidade de vida.
Eventualmente, a medicina reconhece sua incapacidade de tratar a endometriose [B], assim como vez ou outra também admite o quanto a terapêutica da endometriose praticamente não evoluiu [C]. Esquecem, frequentemente, de citar o quanto a abordagem médica dessa enfermidade é agressiva e invasiva.
Mas pesquisas mostram sucessivamente, que a causa é dominância estrogênica.
Vários trabalhos científicos – [E] é apenas um deles – mostram que o tecido onde a endometriose se desenvolve é um local de alta produção de estradiol, de conversão de estrona [E1] em estradiol [E2] o hormônio mais agressivo e mais potente indutor de enfermidades como câncer e endometriose.
O trabalho [E] reconhece que as células da endometriose convertem andrógenos circulantes em estrona que, na sequência, vira estradiol no tecido enfermo atraves da enzima 17betaHSD tipo 1. Isso significa que o produto da ação da aromatase, estrona, que usualmente, é um estrógeno fraco, é convertido no potente 17beta-estradiol nos focos de endometriose.
A progesterona, quem diria, inibe essa enzima, inativando o estradiol, fazendo com que ele se converta em estrona [E]. Conclusão: deficiência de progesterona faz com que o tecido da endometriose não pare de gerar o potente agente da alimentação da endometriose, o 17-beta-estradiol. A óbvia conclusão é de que progesterona - na forma e dose corretas - estaria sistematicamente indicada em endometriose. Ela antagoniza com os estrógenos por essa e por outras vias, como cansou de explicar o PhD R. Peat.
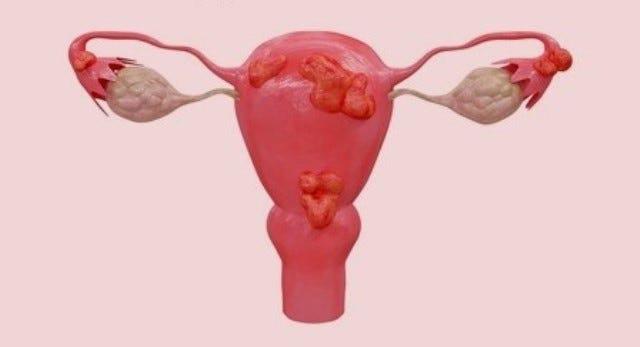
O crescimento do tecido do endométrio fora da cavidade uterina é uma característica da endometriose. Que virá junto com dor, perda da qualidade de vida de mulheres por todo lado. Mas, como enfatiza o trabalho [F] basicamente o que a medicina sabe fazer de mais moderno na endometriose é o uso de inibidores da aromatase... Demonstrando uma enorme e bizarra dificuldade para entender o inteligível: decifrar o papel da progesterona[G], antagonista fisiológico dos estrógenos.
Muitos cientistas não têm nenhuma dúvida: “o estrogênio é o mais importante fator conhecido que estimula o crescimento da endometriose” [G].
Se a mulher não tem endometriose, seu endométrio não expressa a aromatase [J].
E são autores que vão mais longe, reconhecendo que estrogênio promove a síntese de mediadores inflamatórios como as prostaglandinas e que, ao mesmo tempo, na via inversa, qualquer processo inflamatório aciona a enzima que produz estrogênio, a aromatase [G].
Ou seja, o estrogênio é pró-inflamatório e, também por essa via, constrói endometriose.
Outros cientistas também destacam o papel da inflamação crônica por trás da endometriose. Sendo que admitem que essa inflamação aciona a aromatase, que leva ao estradiol. “PGE2 parece ser o mais potente e conhecido estimulador da aromatase na endometriose” [F]. Eis a conexão inflamação-aromatase-estrogênio tão destacada, por R. Peat
O tecido onde se desenvolve a endometriose é de baixa energia e tende a utilizar formas ineficientes de produção de energia. A presença, em excesso, do estradiol é uma indicação indireta disso, na perspectiva de R. Peat. A abordagem terapêutica deveria levar isso em conta. E que, portanto, hipotireoidismo pode ser uma causa fundamental, como também, por outro lado, anticoncepcionais, formas de estresse crônico, deficiências nutricionais [da vitamina A, selênio, açúcar – ativador do hormônio tireoidiano no fígado - por exemplo]. Ou o uso de óleos insaturados, que impulsionam o estrogênio e bloqueiam a tireoide.
Por sua vez, como já deve ter ficado claro, a aromatase aparece, expressada, em qualquer tecido inflamado.
Mediadores inflamatórios, como PGE2, acionam produção de estrogênio. Inflamação estrogeniza o corpo. Estrogênio aparece claramente em um dos seus papeis centrais: hormônio do estresse.
O estrogênio aciona mastócitos, promove dor e inflamação.
A endometriose foi entendida assim por R. Peat há décadas. Mais recentemente, a medicina começa a raciocinar nessa mesma direção, ainda que parcialmente: “Endometriose é uma doença estrogênio-dependente e uma doença crônica inflamatória caracterizada pelo crescimento de tecido endometrial fora do útero”, na qual os mastócitos possuem papel central.
E mais, “a influência do estrogênio na função do mastócito vem sendo reconhecida como um fator condutor potencial de doenças alérgicas e inflamatórias crônicas” [A].
A aromatase está aberrantemente expressa no tecido endometrial doente [endometriose] e sintetiza estrógenos que acionam a enzima ciclooxigenase 2, a qual aumentará os níveis de PGE2, prostaglandina 2. O feed back vicioso continua: a PGE2, por sua vez, é um potente indutor da atividade da aromatase nas células endometrióticas [G].
Estes cientistas foram mais longe e observaram que o tecido da endometriose é deficiente naquela enzima a 17-beta hidroxiestroide desidrogenase tipo 2, a 17beta-HSD.
Isso significa que estradiol continuará sendo produzido copiosamente a partir da estrona [que a aromatase sintetizou] sem impedimento daquela enzima, ausente. Em vez de concluir que aqui entraria, terapeuticamente, a progesterona, os cientistas – por alguma tara cognitiva obscura – basicamente ficam repetindo que “precisamos usar inibidores químicos da aromatase”. Por si só, isso daria um romance sobre um determinado tipo de “cego que não quer ver” ou de juntar os pontos fisiologia-fisiopatologia-estratégia terapêutica.
Outro trabalho [D] reconhece que não dá para ficar usando drogas antiaromatase por muito tempo, por conta de sua toxicidade e, também, porque não curam a endometriose.
E conclui [D] que a medicina precisa abordar a endometriose não apenas procurando aliviar os sintomas. Uma declaração de intenções, mas que não enxerga a progesterona.
Muitos outros continuam repetindo, ano após ano [E] que uma vez que a endometriose deriva da alta concentração local de E2, devemos procurar drogas – a palavra chave talvez seja drogas patenteáveis - que liquidem com esse estrógeno, o estradiol [E2][I].
Mesma ladainha.
Mais reducionista é quase impossível. É mais ou menos como no câncer: o problema a ser erradicado, incinerado e queimado é o tumor, e aí, neste caso, mostram que o terreno, para a medicina não é nada. Que esperar de tal abordagem “teórica”Ɂ
No dia em que a medicina conseguir juntar os pontos, a fisiologia e a fisiopatologia ganharão a dimensão de totalidade [que é sua essência], por mais que a medicina se ocupe, todo o tempo, em fragmentar, fatiar e promover o reducionismo no corpo humano, deixando, assim, de entender a saúde e a doença.
GM Fontes, Brasília, 24-2-24
As informações aqui presentes não pretendem servir para uso diagnóstico, prescrição médica, tratamento, prevenção ou mitigação de qualquer doença humana. Não pretendem substituir a consulta ao profissional médico ou servir como recomendação para qualquer plano de tratamento. Trata-se de informações com fins estritamente educativos.
Referências ______________________
[A] McCALLION A NASIRZADEH Y, 2022. Estrogen mediates inflammatory role of mast cells in endometriosis pathophysiology. Front Immunol. 2022 Aug 9:13:961599. doi: 10.3389/fimmu.2022.961599. eCollection 2022. PMID: 36016927 PMCID: PMC9396281 DOI: 10.3389/fimmu.2022.961599 “Endometriosis is an estrogen dependent, chronic inflammatory disease characterized by the growth of endometrial lining outside of the uterus. Mast cells have emerged as key players in regulating not only allergic responses but also other mechanisms such as angiogenesis, fibrosis, and pain. The influence of estrogen on mast cell function has also been recognized as a potential factor driving disease pathophysiology in number of allergic and chronic inflammatory conditions. However, precise information is lacking on the cross talk between endocrine and immune factors within the endometriotic lesions and whether that contributes to the involvement of mast cells with disease pathophysiology. In this study, we observed a significant increase in mast cell numbers within endometriotic lesions compared to matched eutopic endometrium from the same patients. Compared to eutopic endometrium, endometriotic lesions had significantly higher levels of stem cell factor (SCF), a potent growth factor critical for mast cell expansion, differentiation, and survival for tissue resident mast cells. Targeted mRNA Q-PCR array revealed that the endometriotic lesions harbour microenvironment (upregulation of CPA3, VCAM1, CCL2, CMA1, CCR1, and KITLG) that is conducive to mast cells recruitment and subsequent differentiation. To examine cross-talk of mast cells within the endometriotic lesion microenvironment, endometriotic epithelial cells (12Z) and endometrial stromal cells (hESC) incubated with mast cell-conditioned media showed significantly increased production of pro-inflammatory and chemokinetic cytokines. To further understand the impact of estrogen on mast cells in endometriosis, we induced endometriosis in C57BL/6 mice. Mature mast cells were significantly higher in peritoneal fluid of estrogen-treated mice compared to untreated mice within the sham operated groups. Mouse endometriotic lesion tissue revealed several genes (qRT-PCR) relevant in mast cell biology significantly upregulated in the estrogen treated, endometriosis-induced group compared to control endometrium. The endometriotic lesions from estrogen treated mice also had significantly higher density of Alcian blue stained mast cells compared to untreated lesions or control endometrium. Collectively, these findings suggest that endometriotic lesions provide a microenvironment necessary for recruitment and differentiation of mast cells. In turn, mast cells potentially release pro-inflammatory mediators that contribute to chronic pelvic pain and endometriosis disease progression.
[B] BUGGIO L DRIDI D BARBARA G, 2022. Novel pharmacological therapies for the treatment of endometriosis. Expert Rev Clin Pharmacol. 2022 Sep;15(9):1039-1052. doi: 10.1080/17512433.2022.2117155. Epub 2022 Aug 30. PMID: 36000243 DOI: 10.1080/17512433.2022.2117155 “Introduction: Endometriosis is a chronic, estrogen-dependent, inflammatory disease associated with pelvic pain, infertility, impaired sexual function, and psychological suffering. Therefore, tailored patient management appears of primary importance to address specific issues and identify the appropriate treatment for each woman. Over the years, abundant research has been carried out with the objective to find new therapeutic approaches for this multifaceted disease.
Areas covered: This narrative review aims to present the latest advances in the pharmacological management of endometriosis. In particular, the potential role of GnRH antagonists, selective progesterone receptor modulators (SPRMs), and selective estrogen receptors modulators (SERMs) will be discussed. We performed a literature search in PubMed and Embase, and selected the best quality evidence, giving preference to the most recent and definitive original articles and reviews.
Expert opinion: Medical therapy represents the cornerstone of endometriosis management, although few advances have been made in the last decade. Most studies have focused on the evaluation of the efficacy and safety of GnRH antagonists (plus add-back therapy in cases of prolonged treatment), which should be used as second-line treatment options in selected cases (i.e. non-responders to first-line treatments). Further studies are needed to identify the ideal treatment for women with endometriosis”.
[C] ZAJEC V Mijus M VITALE S G, 2022. Current status and challenges of drug development for hormonal treatment of endometriosis: a systematic review of randomized control trials. Gynecol Endocrinol. 2022 Sep;38(9):713-720. doi: 10.1080/09513590.2022.2109145. Epub 2022 Aug 15. PMID: 35971323 DOI: 10.1080/09513590.2022.2109145 “Objective: The aim of this systematic review is to summarize the data obtained from randomized controlled trials looking at new pharmacologic treatments for endometriosis published over the last decade with a focus on hormonal therapeutic options for endometriosis-associated pelvic pain (EAPP), excluding studies focusing on fertility.
Methods: We identified relevant original studies in the English language through a search of the MEDLINE, Scopus, and EMBASE (2012 to present) databases using the appropriate MeSH terms and applying the article type filter 'randomized controlled trials'. A total of 219 records were found during the electronic search. After a detailed evaluation and review of the manuscripts, 11 primary articles met the inclusion criteria. A systematic review of the data was conducted.
Results: This review included several emerging drug therapies for EAPP. Randomized control trials showed promising results with several oral gonadotropin-releasing hormone antagonists (elagolix, relugolix, ASP1707, linzagolix). However, studies of other hormonal agents such as aromatase inhibitors and selective progesterone receptor modulators have not yielded significant or new advantages. Selective estrogen receptor modulators have not been represented in randomized control trials and have failed to demonstrate clinical efficacy.
Conclusion: Although numerous novel agents are being investigated for the treatment of endometriosis, there is still no significant progress in the development of curative rather than suppressive drugs. Therefore, further efforts are needed to develop an effective and hopefully curative treatment for this chronic, costly, and overwhelming disease”.
[D] Endometriosis and Estrogen – site do FPS – cita vários dos artigos aqui presentes.
[E] ZEITOUN K TAKAYAMA K, SASANO H, 1998. Deficient 17beta-hydroxysteroid dehydrogenase type 2 expression in endometriosis: failure to metabolize 17beta-estradiol.
Clin Endocrinol Metab. 1998. Dec;83(12):4474-80.
“Aberrant aromatase expression in stromal cells of endometriosis gives rise to conversion of circulating androstenedione to estrone in this tissue, whereas aromatase expression is absent in the eutopic endometrium. In this study, we initially demonstrated by Northern blotting transcripts of the reductive 17beta-hydroxysteroid dehydrogenase (17betaHSD) type 1, which catalyzes the conversion of estrone to 17beta-estradiol, in both eutopic endometrium and endometriosis. Thus, it follows that the product of the aromatase reaction, namely estrone, that is weakly estrogenic can be converted to the potent estrogen, 17beta-estradiol, in endometriotic tissues. It was previously demonstrated that progesterone stimulates the inactivation of 17beta-estradiol through conversion to estrone in eutopic endometrial epithelial cells…In conclusion, inactivation of 17beta-estradiol is impaired in endometriotic tissues due to deficient expression of 17betaHSD-2, which is normally expressed in eutopic endometrium in response to progesterone”.
[F] NOTHNICK W B, 2011. The emerging use of aromatase inhibitors for endometriosis treatment. Reproductive Biology and Endocrinology 2011, 9:87
“Endometriosis is defined as the growth of endometrial tissue outside of the uterine cavity. The disease occurs primarily in women of reproductive age but recurrent endometriosis is also detected in post-menopausal women. Regardless of age, endometriosis is associated with pain and reduces the quality of life for millions of women world-wide. Conventional therapies focus on reducing systemic levels of estrogen which results in cessation of endometriotic implant growth and pain symptoms associated with the disease. However, these treatments are not effective in all women and are not without side effects. Based upon the discovery that endometriotic tissue over-expresses aromatase, an enzyme critical for estrogen production, emphasis has been placed upon the use of aromatase inhibitors for the treatment of endometriosis and its associated symptoms. This article will review the rationale behind the use of aromatase inhibitors in treating endometriosis and summarize those studies which have evaluated the use of aromatase inhibitors in the treatment of endometriosis and its associated symptoms.
[G] BULUN S E ZEITOUN K TAKAYAMA K, 1999. Estrogen production in endometriosis and use of aromatase inhibitors to treat endometriosis. Endocr Relat Cancer. 1999 Jun;6(2):293-301. “Estrogen is the most important known factor that stimulates the growth of endometriosis. Estrogen delivery to endometriotic implants was classically viewed to be only via the circulating blood in an endocrine fashion. We recently uncovered an autocrine positive feedback mechanism, which favored the continuous production of estrogen and prostaglandin (PG)E2 in the endometriotic stromal cells. The enzyme, aromatase, is aberrantly expressed in endometriotic stromal cells and catalyzes the conversion of C19 steroids to estrogens, which then stimulate cyclooxygenase-2 to increase the levels of PGE2. PGE2, in turn, is a potent inducer of aromatase activity in endometriotic stromal cells. Aromatase is not expressed in the eutopic endometrium. Aromatase expression in endometriosis and its inhibition in eutopic endometrium are controlled by the competitive binding of a stimulatory transcription factor, steroidogenic factor-1, and an inhibitory factor, chicken ovalbumin upstream promoter-transcription factor to a regulatory element in the aromatase P450 gene promoter. In addition, we find that endometriotic tissue is deficient in 17beta-hydroxysteroid dehydrogenase type 2, which is normally expressed in eutopic endometrial glandular cells and inactivates estradiol-17beta to estrone. This deficiency is another aberration that favors higher levels of estradiol-17beta in endometriotic tissues in comparison with the eutopic endometrium. The clinical relevance of local aromatase expression in endometriosis was exemplified by the successful treatment of an unusually aggressive form of recurrent endometriosis in a postmenopausal woman using an aromatase inhibitor”.
[H] FEDELE L BERLANDA N, 2004. Emerging drugs for endometriosis. Expert Opin Emerg Drugs. 2004 May;9(1):167-77.
“Medical treatment of endometriosis relies on drugs that suppress ovarian steroids and induce an hypoestrogenic state that causes atrophy of ectopic endometrium. Gonadotrophin-releasing hormone (GnRH) analogues, danazol, progestogens and oestrogen-progestin combinations have all proven effective in relieving pain and reducing the extent of endometriotic implants. However, symptoms often recur after discontinuation of therapy and hypoestrogenism-related side effects limit the long-term use of most medications. Furthermore, these therapies are of limited value in patients with a desire to become pregnant because they inhibit ovulation. An important target for current research is to identify effective therapies that can be safely administered in the long term. GnRH analogues with add-back therapy, progestogens and continuous oral contraceptive are options available for a medium or long-term systemic treatment. Mifepristone, an antiprogestogen, may constitute an alternative if encouraging preliminary data on its effectiveness and tolerability are confirmed. A very appealing area of interest is the possibility of treating endometriosis without suppressing ovarian function. Aromatase inhibitors might have such characteristics as they have been shown to inhibit oestrogen production selectively in endometriotic lesions, without affecting ovarian function; the clinical role of these drugs in the treatment of endometriosis is under evaluation. Levonorgestrel medicated intrauterine device has proven effective in relieving dysmenorrhoea associated with endometriosis, as well as pain associated with rectovaginal endometriosis. Although a systemic absorption is present determining side effects, this approach is promising in the long-term management of this condition. A fundamental objective of research in endometriosis treatment is to develop new therapeutic approaches based on the findings from experimental studies on the aetiopathogenesis of the disease; current research is focusing on anti-inflammatory drugs and modulators of the immune system. TNF-binding protein-1 and IL-12 have proved effective in reducing endometriotic lesions in animal models, while pentoxifylline and INF-alpha 2b have shown encouraging results in clinical studies. This area may be of paramount importance in the near future in order to develop a therapy that could prevent or eradicate endometriosis rather than merely relieving the symptoms”.
[I] ZEITOUN K M BULUN S E, 1999. Aromatase: a key molecule in the pathophysiology of endometriosis and a therapeutic target. Fertil Steril. 1999 Dec;72(6):961-9.”
OBJECTIVE: To provide a clinically useful model illustrating the molecular aberrations affecting estrogen biosynthesis and metabolism in endometriosis and to discuss the therapeutic role of aromatase inhibitors.
DESIGN: Literature review.
RESULT(S): Several molecular aberrations were found in endometriotic lesions (in contrast to eutopic endometrium) that favor increased local concentrations of E2. Endometriotic stromal cells aberrantly express aromatase, which converts C19, steroids to estrogens. Aromatase activity in these cells is stimulated by prostaglandin (PG)E2. Estrogen stimulates cyclooxygenase-2, giving rise to increased PGE2 formation. Thus, this positive feedback loop produces increasing quantities of E2 and PGE2 in endometriosis. The lack of aromatase expression in eutopic endometrium is maintained by binding of an inhibitory transcription factor, COUP-TF, to the aromatase promoter. In endometriosis, however, an aberrantly expressed factor, SF-1, displaces COUP-TF to bind to this same promoter and activates aromatase expression and thus local estrogen biosynthesis. Additionally, endometriotic glandular cells are deficient in 17beta-hydroxysteroid dehydrogenase type 2, which converts E2 to estrone in the eutopic endometrium in response to P. Deficiency of this enzyme in endometriosis impairs the inactivation of E2 and may be a consequence of insensitivity to P.
CONCLUSION(S): Molecular aberrations that increase local E2 concentrations may be important in the etiology of endometriosis. These molecules may be targeted to develop novel therapeutic strategies. The clinical relevance of aromatase expression in endometriosis was shown recently by the successful treatment of an unusually aggressive case of postmenopausal endometriosis with use of an aromatase inhibitor”.
[J] NOBLE L S TAKAYAMA, 1997. Prostaglandin E2 stimulates aromatase expression in endometriosis-derived stromal cells. J Clin Endocrinol Metab. 1997 Feb;82(2):600-6. “C19 steroids are converted to estrogens by aromatase P450 (P450arom). Aromatase expression in humans is regulated by use of tissue-specific promoters in the placenta (promoter I.1), adipose tissue (promoters I.4, I.3, and II), and gonads (promoter II). The use of each promoter gives rise to a population of P450arom messenger ribonucleic acid (mRNA) species with a unique untranslated 5′-terminus. Aromatase is not expressed in the endometrium of disease-free women. We demonstrated, however, the presence of P450arom mRNA in pelvic endometriotic implants and eutopic endometrial curettings of women with endometriosis. In the current report, aromatase activity and P450arom gene expression were investigated in cultured stromal cells derived from eutopic endometrium and ovarian endometriomas of women with pelvic endometriosis. We also investigated the hormonal regulation of aromatase expression and alternative promoter use in these cells. The effects of interleukin-1 beta (IL-1 beta), IL-2, IL-6, IL-11, oncostatin M, IL-15, tumor necrosis factor-alpha, PGE2, estradiol, R5020, dexamethasone, and dibutyryl cAMP (Bt2cAMP) on aromatase activity in endometriosis-derived stromal cells were assessed. We chose treatments with PGs and ILs because of the inflammatory nature of endometriosis. PGE2 stimulated aromatase activity in endometriosis-derived stromal cells by 19- to 44-fold (37-221 pmol/mg protein-4 h), whereas Bt2cAMP induction was 26- to 60-fold the baseline level. No stimulation was observed by estradiol or R5020 or by IL-1 beta, IL-2, IL-6, IL-11, IL-15, or TNF alpha in the presence or absence of glucocorticoids. A modest induction of aromatase activity (2-fold) was observed in dexamethasone- plus oncostatin M-treated cells. These changes in aromatase activity were accompanied by comparable changes in the levels of P450arom mRNA levels, determined by a quantitative reverse transcription-PCR method. Promoter-specific 5′-ends of P450arom transcripts in total RNA from endometriosis-derived stromal cells treated with PGE2 and Bt2cAMP were amplified employing a novel modified rapid amplification of cDNA5′-ends/Southern hybridization method using exon-specific oligonucleotide probes. The majority of P450arom transcripts in these cells contained the gonadal-type promoter II-specific sequences, whereas very few transcripts contained adipose-type promoter I.3- and I.4-specific sequences. PGE2 appears to be the most potent known stimulator of aromatase in endometriosis. Aromatase expression in PGE2-stimulated stromal cells of endometriosis is regulated primarily by the classically located promoter II, which, in turn, is regulated by cAMP. As PGE2 is known to increase intracellular cAMP levels, estrogen biosynthesis in endometriosis may be primarily regulated by PGE2 that is locally produced. Consequent local estrogen production may promote the growth of endometriotic implants”.
[K] FERRERO S VENTURINI P L RAGNI N, 2009. Pharmacological treatment of endometriosis: experience with aromatase inhibitors. Drugs. 2009 May 29;69(8):943-52. doi: 10.2165/00003495-200969080-00001. “Current treatment of endometriosis is mainly based on surgery and ovarian suppressive agents. In the last 10 years, it has been demonstrated that aromatase P450, a key enzyme for estrogen biosynthesis, may have a pathogenic role in endometriosis because it is aberrantly expressed in endometriotic implants and in eutopic endometrium of women with endometriosis. Therefore, inhibition of aromatase activity may represent a new therapeutic option for endometriosis. Case reports and observational studies have shown that pain symptoms caused by endometriosis quickly improve after administration of aromatase inhibitors. Limited data are available on the long-term course of pain symptoms after completion of treatment with aromatase inhibitors; however, some recent studies suggest that symptoms may recur at short-term follow-up. A range of results are reported on the effects of aromatase inhibitors on endometriotic lesions, with some authors describing improvements and other authors reporting persistence of pelvic lesions at second-look laparoscopy after treatment. No severe adverse effect has been reported during treatment with aromatase inhibitors both in pre- and postmenopausal women. On the basis of the available data, administration of aromatase inhibitors should now be offered only to the small number of women who have severe pain despite previous surgical and hormonal therapies. Further research in the form of randomized controlled trials will be required before recommending the routine use of these agentes”.
***

Excelente! Minha mulher sofre com endometriose. Você poderia indicar algum médico com essa visão, aqui em Brasília, com quem ela poderia se consultar?