New Hope, for OCD, Is Insurance Covered*, Thanks to This Very Persuasive Newsletter
Evernorth Behavioral Health, as of September 15th, covers dTMS for OCD, and I am completely serious and not at all kidding that it is all thanks to this very newsletter and no one else.
TL;DR the title is making fun of me. But Evernorth, formerly CIGNA, now covers dTMS for OCD!
To be clear, I didn’t do it. It’s been a heroic team effort that took industry1, professional society committees2, payers,3 doctors4, patients5, researchers,6 and even journalists7, all working together. I had a tiny part in the story. Yes, it’s a joke about me being a big narcissist. Yes, I understand people think that.8 No, I don’t believe it to be accurate—I was worried so I asked my psychiatrist to check several times.9 No, I don’t take it as an insult! NPD is a real and serious illness, about which I have contributed scholarly work! Yes, there is some truth to me being a little… confident. I’m a good enough physician.10 This part was supposed to be short!11 C’mon, meta-commentary in my head, let’s stop stalling and write this piece about obsessing already…12
Welcome to Our Keeping up With the News Column for This Week!
In the August 2nd, 2022 article I wrote addressing prior-authorization denial for theoretically experimental and unproven treatments, I made a strident argument which is:13 It is unethical to continue to request more data after FDA clearance for feigned dubiousness about efficacy. The specific treatment I’m referring to here (deep TMS)14 involves brain stimulation15 that is non-invasive16 and causes no permanent changes in brains, and is still the most effective biological treatment17 for obsessive compulsive disorder.
TMS works by creating pulsing, strong magnetic fields that can cause neurons in your brain to fire in a new pattern. This new rhythm of firing interrupts the repetitive thought neural circuit18—this circuit tortures people with obsessions.
We should define what we mean by OCD, for all of my dear readers:
But I’m Messy! I Can’t Have OCD!
OCD, it’s not just hand washing. It’s awful. People can not-stop-thinking-about-it. This is more than just “being contaminated and washing your hands.” It’s thoughts like: “what if I killed someone? What if I am a secret serial killer?” Or even “I might rape that child…what if I’m a pedophile?!”—psychopath serial killers or pedophiles don’t worry about those things. They are, in a way, free of doubt. They may have other problems, but they know for sure who they murdered and that they are sexually attracted to kids. They are not in doubt. OCDBrain is, in the worry and doubt checking game, like most people are when they check their phones:
Imagine if every time you checked your phone it wasn’t to see if you missed a text…
It was to make sure you hadn’t murdered someone. That’s crazy. Of course you didn’t. BING. Let me check one more time. Phew. I guess I di—BING—maybe one more che—BING—I could go back home to double ch—BING. 8, 10, 22, all Hours of the day. Every day. All day. Nearly all the—BING—time. BING. BING. Wait, did I miss a message? I’ll just casually ch—BING.
And, perhaps, the most horrifying version of this is for people with “Harm OCD”, where sufferers become obsessed with suicide. Or, with the worry that they might complete suicide. Horrible images barge into your head, unbidden:
“EAT GLASS.”
“Hang yourself, there is rope, do it, hang yourself hang yourself hang hang HANG.”
“If you’re not careful enough…”
“How can you be so sure you won’t stab yourself in the neck with that pen? Maybe you should just go to the hospital, just in case you might?”
Even if you didn’t personally want to die at all, and you like your life otherwise, these sorts of thoughts-you-can’t-shake-for-hours are profoundly disturbing. The “compulsive” symptoms are not the real story of OCD. Other people can see them, so they get a spotlight. They are a way to reduce the distress of thinking about awful things, if only for a few seconds. This is what coping looks like when you brain has a horror show on repeat. Obsessions, they are the core. People regularly suffer for years and have no idea this is not what other people are also doing in their heads too. They can be in their 60s before they timidly admit “I know it sounds crazy BUT…” to their psychiatrist. And maybe that is a year into treatment. Or more. Or never. Who wants to admit to thinking about hurting children? Thought crimes aren’t real… except to people with OCDbrain, quietly condemning themselves for their evil, criminal, secret psychopath thoughts.
No wonder 14% of people with OCD will attempt suicide at least once. Death-to-suicide rates in OCD are shown to range from 0.7% to 1.4% .
This compares horrifically to other illness in terms of suicide risk (we measure these in “per 100,000”). The base rate in the population, per the World Health Organization is 10.7/100,000.
OCD, in these terms, has a completed suicide rate of 700-1,400/100,000.
To compare, in depression, it’s 214/100,000. Borderline Personality Disorder is a leader, at around 5,000/100,000, and schizophrenia at between 5000-14000/100,000. In bipolar disorder, in a 20 year follow up by Jamison and Goodwin19, it was 9,800/100,000. Eating disorders are higher still.
Yes, you read that correctly. OCD is more lethal in amount of death due to suicide than Major Depression. It’s also more common, and they both suck. But still. It’s almost an order of magnitude more lethal. (Reference here, in body text, because this is such a major claim: The Epidemiology of Suicide by Silke Bachmann, Int J Environ Res Public Health. 2018 Jul; 15(7): 1425.)
The Most Annoying Symptom
“Reassurance seeking”—checking with other people over and over—is a compulsion. For realZ. “Did I offend you? Are you sure? Totally sure? But like… really? …cause…. are you sure?” That is OCD till proven otherwise… it turns out. In the milieu of a psychiatrists office, when someone says, laughing, “I’m kind of OCD about that” it’s because they (very often) absolutely have actual OCD. That is the “kind of” problem that is among the most common thing I see in 60,000+ hours of clinical practice.
And Now We Understand OCD, Back to Insurance!
The backstory on this payer decision has a lot to do with the fact that I’ve been working on this particular issue since the before H7 BrainsWay treatment first came to market in 2018. In the week before I published the article about this treatment, a prior authorization conversation actually happened. And my article changed all that.20 Now:
“Cigna will be issuing an updated revision to its TMS medical coverage policy effective September 15, 2022, extending coverage to patients aged 18 and older diagnosed with OCD. Under the revised policy, an initial 30-36 TMS treatment session regimen21 will be classified as medically necessary after a failure of two or more medication trials and a trial of evidence-based psychotherapy without significant improvement in symptoms. Patients with 30% or greater improvement in their Yale-Brown Obsessive Compulsive Scale (Y-BOCS) maintained for at least two months would also be candidates for an additional regimen of 30-36 sessions.”
This is a sea change for what I consider to be the new gold standard in obsessive compulsive disorder treatment, especially for those who have not responded to traditional treatment. The treatment existed before, but would’ve cost tens of thousands of dollars out of the pockets of people—who in some cases can’t work anymore because they are paralyzed by OCD.
Further data is coming, but we know that greater than half of patients (58%) with treatment resistant OCD (trOCD) get a 30% or greater reduction in symptoms. We are publishing, in the future, an open label data, demonstrating that around 20% of patients can get to remission of their OCD symptoms. When this treatment is done in an accelerated fashion, similar to the FDA clearance of Stanford accelerated intelligent neuromodulation treatment (SAINT), which I wrote about last week, 20% of patients still get to remission in only five days. This data needs to be replicated in sham controlled studies, but likely not large ones. There’s very low placebo response in trOCD, which is not true in studies about medications for first time treatment of OCD.
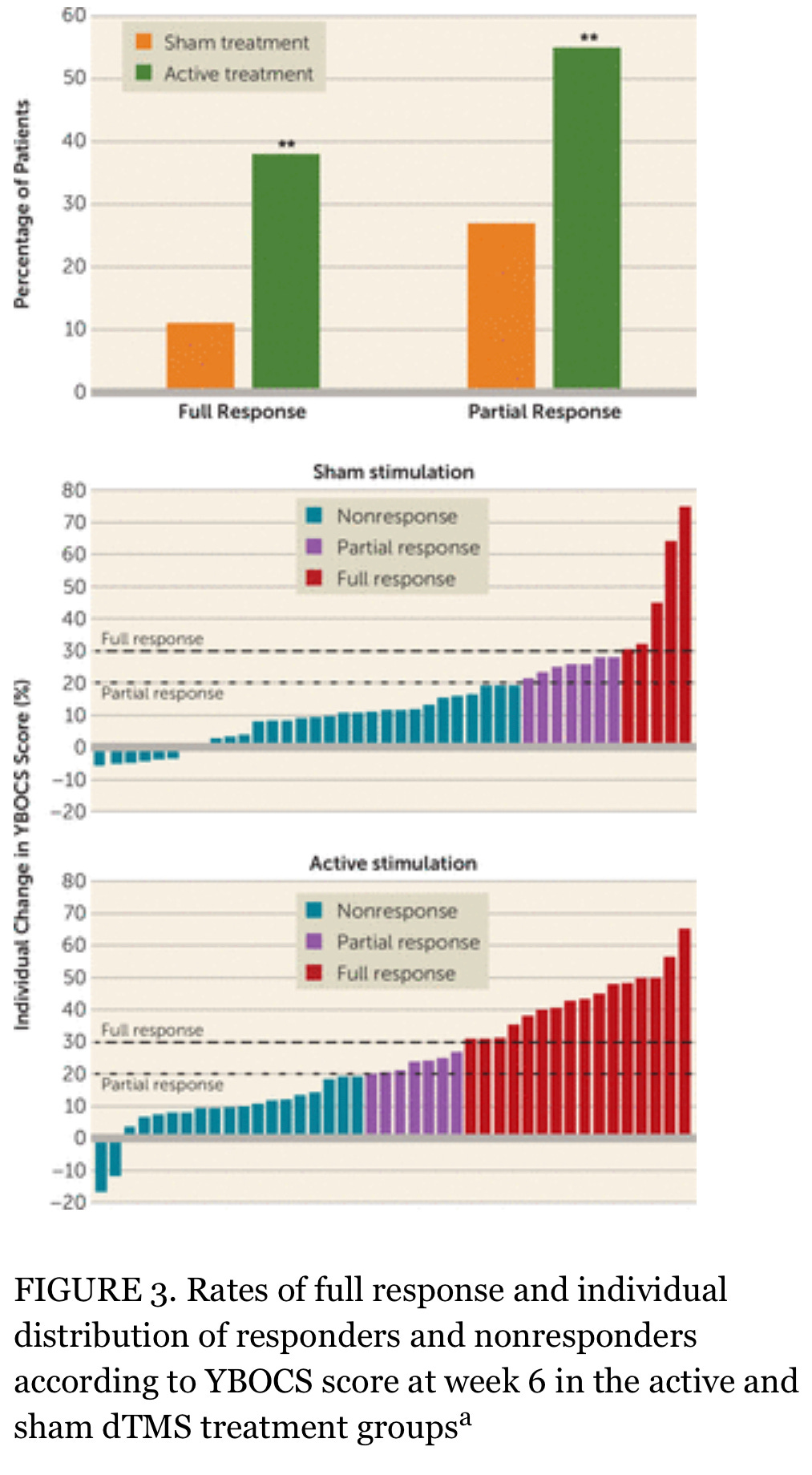
I’m gonna interpret the above graph with you, so it makes sense. This is data from the approval trial for dTMS for OCD with the H7 coil made by the brilliant humans at BrainsWay.
An aside:
Between Dr. Nolan Williams at Stanford and Drs. Abraham Zangen and Aron Tendler, of course with many other collaborators,22 I think we have a few Nobel Prize candidates in psychiatry again, finally!
Everyone in the study had OCD that hadn’t responded to another treatment. That’s why there are so many centers and doctors involved in the trial. For just 99 people, they had to enroll the right 99 people. These 99 people absolutely had to have treatment-refractory illness. The risk that they would respond to a sham treatment was demonstrated to be extremely low. Full response to sham treatment happened in less than 10% of individuals. I’m not biased against partial responses in the real world, but it’s kind of a red herring in research. We want to know if this treatment is biologically active! So, what we wanna look at primarily is how many people who have the problem we think they have—treatment resistant OCD—have a different response profile to the active treatment than to the sham treatment (sham is the placebo of device studies). As we can see in the bottom two graphs, in the sham group, only about four patients met criteria for a full response (>30% symptom reduction) and in the active treatment group, it’s just under 40%!
I Think I’m Feeling Better…? This Pill, It Tastes Just Like a Tic-Tac!
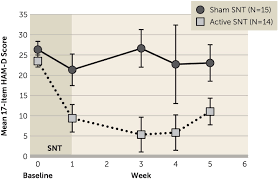
Scientific research is as much about the selection of your research sample as it is about the intervention. For this study to work, the patients needed to have a low placebo response rate. This was predicted by virtue of their prior non-response to treatment. This is the same approach that Drs. Cole and Williams and colleagues took at the Stanford brain stimulation lab when designing the randomized controlled trial for SAINT. Their average number of failed medication trials in depression was 13. In popular language, these are people for whom nothing worked. In the lives of the people suffering vastly, nothing had worked. If you can imagine how hard it is to convince someone who has already had 13 rounds of different depression treatments to try the next thing in a research study, because maybe this time something will help, you get a sense of how difficult that study enrollment can be!
This is what happens when you study people who are very, very unlikely to get better with placebo:
Sorry, I don’t know what’s wrong with me today, that’s not the right picture, that’s just a very good visual metaphor of what their data visualization showed:
Although, honestly, in the future, I may just use this graphic:
A partnership between an insurance payer—Evernorth—and my former practice allowed for us to treat many more people with dTMS for OCD than was possible without the ability to optimize prior authorization workflow. This led to the data collected after dTMS for OCD came to market. This data, along with that from other practices where it was cash pay only, showed that not only did dTMS perform well in study populations, but in the real world. It’s an excellent treatment.23
Today, with that information available to the world, the team at EverNorth were able to use that data to revise their coverage policies. FDA clearance of devices is important. However, coverage policies are more important for patients. If it’s covered, you don’t need to also be rich to get effective treatment. If that coverage isn’t a hassle, it’s even better. We are still not past prior authorization, nor are we past every hurdle for everything. But this is a remarkable step in the right direction, and I’m deeply grateful to everyone involved for working with such good faith towards the outcome. Or, as a meme might put it:
Onward!
—O. Scott Muir, M.D.
Special mention to Scott Blackman, Chris Von Jako, Aron Tendler, Maoz Lev, and so many others at BrainsWay.
The Clinical TMS Society insurance committee does crucial work, with special mention for Baron Short, M.D. and Carlene MacMillan, M.D, co-chairs.
Particularly the team at Evernorth including CMO Doug Nemecek MD, MBA, and countless other folks in provider contracting who I won’t name for their privacy —but thank you AP, ZW, and so many others, from the bottom of my heart.
There are so many doctors who aren’t just working in industry who push the field forward like Joshua Bess, M.D., Robert McMullen, M.D., Padam Bhatia, M.D., Amanda Tinkleman, M.D., Michael Dulchin, M.D., David Carreon, M.D., Sandya Prashad, M.D., Manpreet Singh, M.D., and so so many more.
(The most important group I can’t name)
Like Elinor Cole, Ph.D., Michael Milham, M.D., Abraham Zangen, M.D, Shan Siddiqi, M.D., Eric Hollander, M.D., Wayne Goodman, M.D., and a zillion more.
Journalists like David Adam, and PJ. Vogt:
No, I don’t have OCD.
That confidence doesn’t extend to competent copy editing, clearly.
Can I just check one more thing?
I referenced Nazi Nightmare Dr. Joseph Mengle in the piece. Strident—but not inaccurate. We have medical ethics codified because before that, Monsters like Joseph Mengle torture twin children to learn who would die sooner. Research must be held to the highest ethical standards, which includes not allowing research on human subjects to answer trivial questions. Horrible things are done to vulnerable people when we don’t. Yes, it makes research harder. That is a fair trade off for human subjects protection. I’ve been a research subject. It’s why I’m a psychiatrist now.
Brain stimulation means we can use a changing magnetic field to change how your neutrons fire in your brain, and if you do it repeatedly over many session your brain learns the lesson like you can learn facts from flash cards. You will remember “having fewer OCD symptoms” for a while, but not forever, probably.
No cutting, no meds, it’s like a hummingbird or woodpecker on your baseball helmet kinda feeling.
Pills included.
The brain circuit is called the cortico-striato-thalimo-cortical circuit and It looks like this anatomically:
and like this functionally on a fMRI brain scan:
and when you make it a schematic it looks like this:
and when you map it out on a connectome map (which looks at a stylized version of brain connections) it looks like this:
All of which is to say brain circuits are complex but real and understanding how to readjust them is hope for millions of people who have been denied it by simplistic things like this:
Sorry wrong picture, overly simplistic things like this:
With some subsequent debate. By Kay Jamison herself, of course.
This is of course almost completely false. I might have to check. Can you worry about a good thing you did? That might—you get the point.
This 30-36 number is a minor miracle— in that the initial study only included 29 sessions, and although going past this number is often extremely helpful, usually payers are using that initial study to limit anything they’ll pay for. What this means is that CIGNA actually reviewed the subsequent post-marketing data, found it compelling, and agreed to pay for more than the initial study protocol because it works better some of the time. At this point, if there wasn’t angel trumpet sound effect, it would be appropriate. It also means people don’t have an incentive to say the treatment is for depression instead to get more treatments approved, which is also worth the investment in a couple extra treatments if you care about the veracity of data.
To give the audience a sense of how many people are involved in just one relatively small randomized controlled trial, this is the academic affiliations of the authors on the paper for the FDA clearance of deep TMS in OCD:
The School of Psychological Science, Tel Aviv University, Tel Aviv, Israel (Carmi); the Department of Life Sciences and the Zlotowski Center for Neuroscience, Ben-Gurion University of the Negev, Beer-Sheva, Israel (Carmi, Barnea-Ygael, Roth, Zangen); Advanced Mental Health Care, Inc., Palm Beach, Fla. (Tendler); the Department of Psychiatry and Biobehavioral Sciences, University of California Los Angeles, Los Angeles (Bystritsky); the Spectrum Neuroscience and Treatment Center, New York (Hollander); the Temerty Centre for Therapeutic Brain Intervention and the Campbell Family Research Institute, Centre for Addiction and Mental Health, and the Department of Psychiatry, University of Toronto, Ontario (Blumberger, Daskalakis); the Department of Psychiatry, University of Florida, Gainesville (Ward); the Department of Psychiatry, Northwell Health, New York (Lapidus); the Department of Psychiatry and Behavioral Health System, Icahn School of Medicine at Mount Sinai, New York (Goodman); the Lindner Center of HOPE, Mason, Ohio (Casuto); the Department of Psychiatry and Behavioral Neuroscience, University of Cincinnati College of Medicine, Cincinnati (Casuto); the Department of Psychiatry, University of California San Diego, La Jolla (Feifel); the Sackler Faculty of Medicine, Tel Aviv University, Tel Aviv, Israel (Zohar).
Greater than half of people get 30% or more better even outside of a research study, where most treatments perform a worse than the lab!